Widgetized Section
Go to Admin » Appearance » Widgets » and move Gabfire Widget: Social into that MastheadOverlay zone
Structural Racism is a Growing Public Health Concern: Time to Disrupt the Status Quo
The views expressed are those of the author and do not necessarily reflect the views of ASPA as an organization.
By Vanessa Lopez-Littleton and Carla Jackie Sampson
June 29, 2020
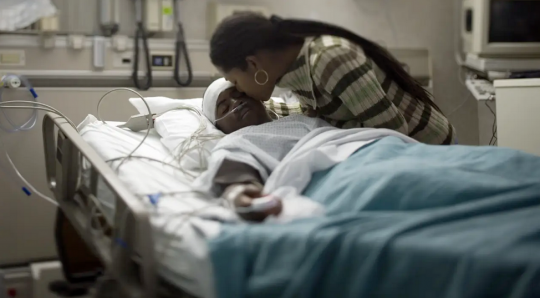
Structural racism is hardwired into American public policy and has a deleterious effect on the health status of Black people. Poor Black health outcomes are the manifestation of the lack of equal opportunity and the denial of full citizenship rights dating back to before the passage of the Emancipation Proclamation, and even since the passage of the Civil Rights Act of 1964. Today, the state of Black health in the United States, one of the most affluent countries in the world, is a growing public health concern. In our upcoming book chapter, we identify structural racism as a risk factor for adverse health outcomes and call for racism to be identified as a social determinant of health. No longer is it appropriate to mask racism by making it synonymous with discrimination, an oft inconsequential legal term that serves as a barrier to accessing the rights and freedoms of full citizenship for Black Americans.
While Black people in the United States face a disproportionate burden of illness, injury, death and disease, the death of any child before their first birthday is one of the most troubling and often preventable outcomes. As such, infant mortality rates are often used as a sensitive barometer of the health of a community. In 2017, the Black infant mortality rate of 11.0 (deaths per 1,000 live births) was nearly three times the rate of the White infant mortality rate (4.7) and on par with countries such as Turkey and Libya. In much the same way, Black women are dying in childbirth at an alarming rate. In 2018, Black women died in childbirth at a rate of 37.1 (deaths per 100,000 live births), while White women only experienced a rate of 14.7. These indicators point to deeply troubled systems in the United States. One social. One healthcare. Both underscored by structural racism.
To be Black in America is to be saddled with a legacy of oppression and subjugation that extends beyond our existence and engulfs a deeply complex chasm that divides American life and the American dream. But not since the Civil War has this nation so openly grappled with manifestations of racism. The killings of George Floyd, Breonna Taylor, Ahmaud Arbery and Rayshard Brooks, and the experience of Christian Cooper in New York City’s Central Park offer a sobering reality of the perils of being Black in America. Social protests around the world are fueled by the seemingly unabated procession of killings by law enforcement officers. These killings are tantamount to human rights violations—abuses to the security of a person by state actors. Law enforcement officers should be peace officers, but that notion has been corrupted by an assault on the civil liberties of Black Americans by “a few bad actors.”
The challenge of rooting out those perpetrators has become a nebulous idea since those actors are part of a system that is responsible for policing itself. While we should reject the conclusion that there is something sinister about law enforcement as a whole, we must wonder if the system that shields bad actors behind a blue wall of silence is somehow complicit in the systematic oppression of Black citizens and the plethora of consequences that follow. As a result of their actions and inactions, police violence is a growing public health concern.
In addition to the risk of police violence, Black citizens across the United States are disproportionately affected by serious illnesses, including COVID-19. Since COVID-19 was declared a national emergency less than four months ago, today more than 124,000 United States citizens have died from COVID-19. According to the CDC, Black people are at a greater risk for COVID-19 and other illnesses based on their living and working conditions, as well as their individual health circumstances. For the past two decades, public health officials have known about the social determinants of health and understood that where you live, work, play and worship matters in terms of health risks and outcomes. Yet, there has been a persistent inability to translate this knowledge into saving lives, particularly Black lives.
The disparate impact of COVID-19 on the Black community is deeply troubling and points to a flaw in the public health system. In much the same way, police violence and persistent disparate health outcomes serve as further evidence of broader systemic ills, including structural racism. But detangling the relationships among the social determinants of health is a challenge in a society built on a White racial frame—the dominant lens.
Now that racism is finally being recognized as an entrenched public health concern, we must begin to intentionally disrupt the status quo by acknowledging that racism is inherent in all public policies and work assiduously to dismantle those systems. Now is the tipping point for the identification of the perils of the White racial frame. Now is the time to reject color-blind and race-neutral policy approaches. Now is the time to remove all barriers to the rights and freedoms of full citizenship for all Black Americans.
Authors:
Vanessa Lopez-Littleton, Ph.D., RN, is an Associate Professor in the Department of Health, Human Services, and Public Policy at California State University, Monterey Bay. Her research interests include social equity, health disparities, racial equity, and cultural competence. She may be reached at [email protected], DrVLoLil.Com or @DrVLoLil
Carla Jackie Sampson, Ph.D., MBA, FACHE, is a Clinical Associate Professor and Director of the Health Policy and Management Program and online Master of Health Administration Program at NYU’s Robert F. Wagner Graduate School of Public Service. Her research interests include healthcare workforce policy, social determinants of health, and anchor mission strategy development. She may be reached at [email protected] or @ProfessorSamps1
